Jenson Stephen Peter – 5 November 2022 / 30.5 weeks – Wellington hospital, as told by mum Zoe
As I share Jensons birth story, Jenson is currently bulldozing around the lounge, as a rambunctious, charmingly cheeky, food monster one year old.
Jenson was a special baby right from the get go. I suffer from endometriosis so falling pregnant without a clear out surgery was surprising to not just me, but also my doctors. Everything seemed to be going normally until a 23 week checkup with my midwife, when she took my blood pressure it was high enough to warrant concern. My midwife called the Hutt hospital and they wanted to monitor me and baby and see if this was a one off or something more serious. Little did I know this was going to become our new normal.
I was admitted into Hutt hospital for three nights to monitor and trial medication. Since there is a history of high blood pressure and pre-eclampsia in my family, the team at the Hutt wanted regular twice a week blood tests and blood pressure monitoring at the hospital, as well as my usual midwife appointments. For the next seven weeks at least once a week, I was being admitted into Hutt hospital as my blood pressure was usually sitting at over 185/95 , and the combination of meds didn’t seem to be controlling my BP for more than five days at a time. The most frustrating part was I felt fine. I didn’t have any of the usual symptoms of pre-eclampsia or high blood pressure other than the occasional flashing stars in my vision.
The team at Hutt had briefed me that Jenson would be a premature baby, and they hoped to get me and baby boy past 28 weeks gestation. I was having scans every two weeks from 26 weeks to monitor how the blood pressure was impacting Jenson. At my 30 weeks scan was when everything changed. All was going well until we got to the measurements of baby’s stomach. Then the scan ended rather quickly, and we were told they would contact my midwife and here was the code to see pictures of our baby. Within 15 minutes of the scan ending, I had a call to go straight to Hutt Hospital, as babys stomach was in the second centile and had stopped growing.
My blood pressure was sky high and the doctors made the call to admit me and start steroid injections. This all happened on Wednesday afternoon and on Friday I woke up and knew something wasn’t right. I couldn’t tell the doctors exactly what it was, but I just knew something wasn’t right with my body and my baby. Saturday morning I woke up and felt worse, but one of the morning doctors told me he felt I would make it to 34 weeks. I was 30.5 weeks, this was the day our boy was born. At 11.30am that same morning, I got severe pain on my right side, it felt like I couldn’t breathe. The medication to get my blood pressure down was no longer working, my leg muscles were constantly spasming and the Drs felt I was starting to have seizures. Hutt hospital could deliver my boy but they could not look after him as he would be under 32 weeks. I was told I was going to be transferred into Wellington hospital by ambulance that afternoon and to be prepared for an emergency ceaserean.
Once in Wellington we were told by the registrar that we were looking 24-48 hours before we meet our wee boy, however when the boss on duty came to examine me, she decided it was “go time”. My symptoms and blood pressure were worsening, however the only blessing was our boy was still super calm and was not in distress.
When the decision was made it all happened very fast. I was very anxious but the staff in theatre were amazing. They put myself and my partners mind at ease, and we knew myself and our boy was in the best possible hands. At 7.40pm our boy was born. He weighed 1.514kgs which was 500 grams more than doctors had predicated. It seemed all a total blur. All I wanted to hear was my boy cry. When they got him on the table, he cried. Relief. He was as well as could be expected, and didn’t need to be intubated.
I finally got to lay eyes on my first child and touch him for a brief minute before he was wheeled away to NICU. My partner went with him and within 10 minutes the busy theatre seemed empty.
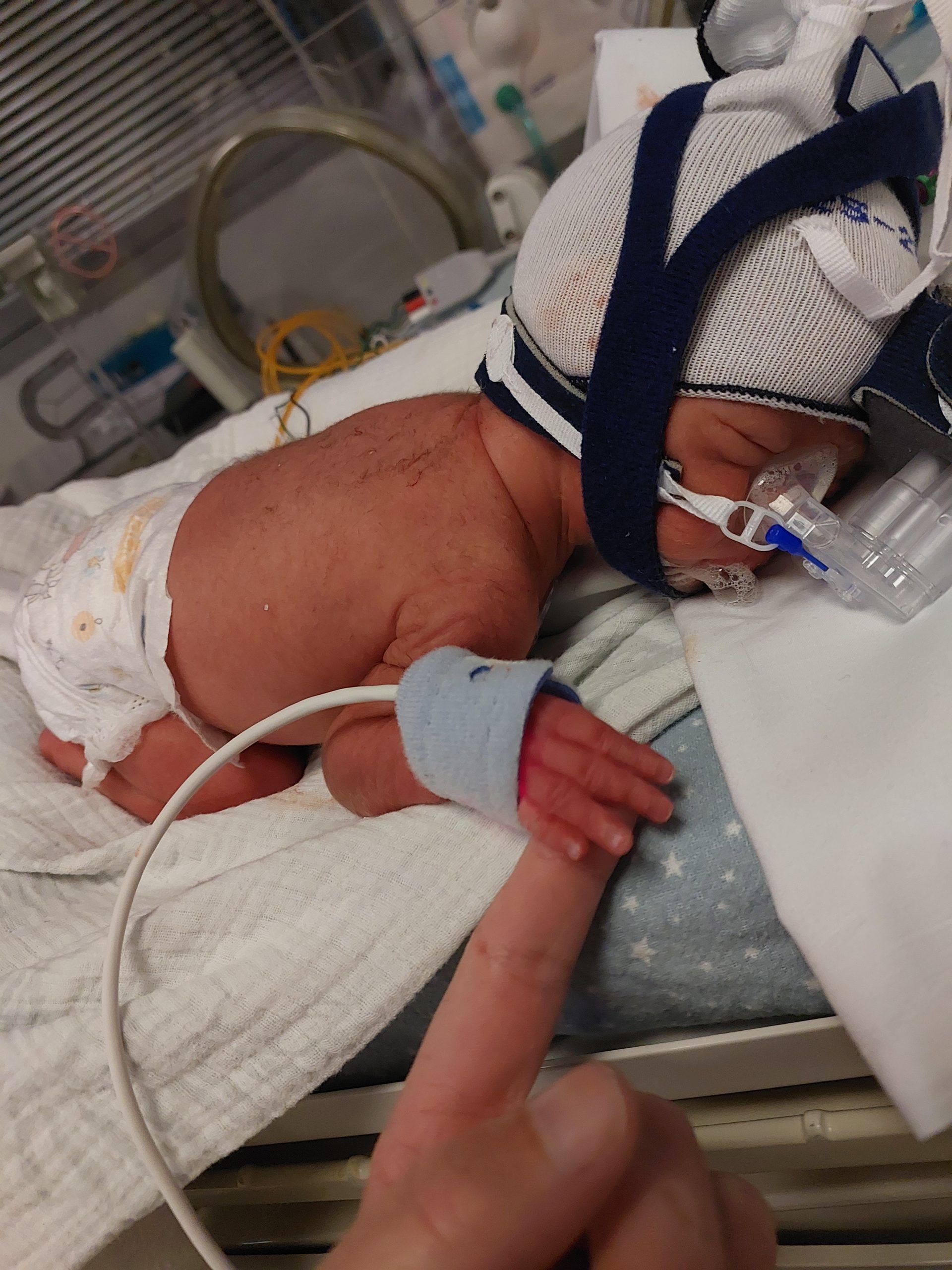
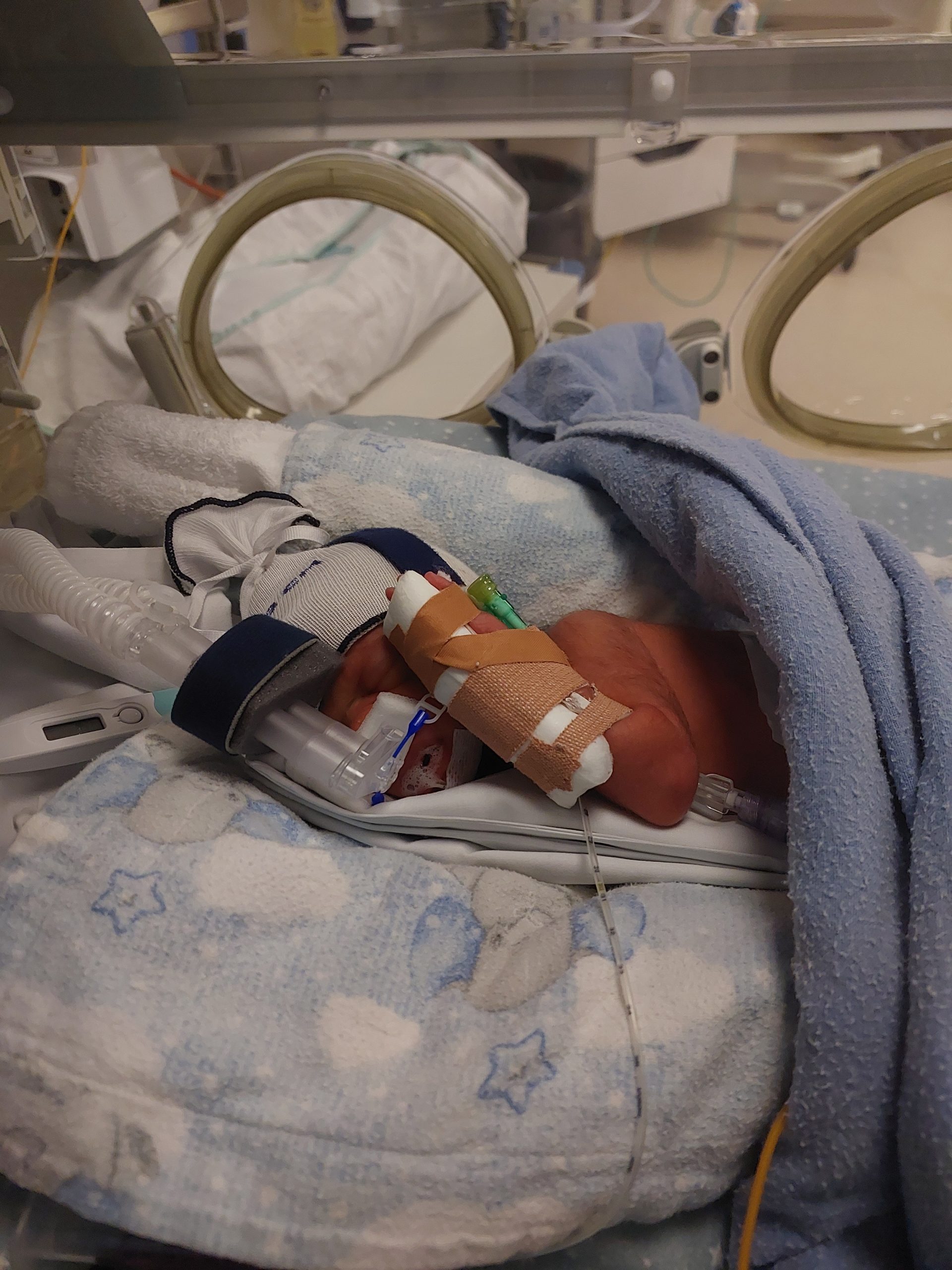
Two hours after he was born, I finally got to properly meet my boy. Being wheeled into NICU still in my bed, was surreal. It seemed so big, and how would I remember where to find my baby. Soon it became so easy to navigate and less intimidating. Our boy seemed so tiny, he had long gangly legs’ and arms, that looked like sticks. It was so overwhelming to take in everything that was happening, what our boy was needing help with, and the gentle intimidation of room E of NICU. However when I held his hand, everything going on around me just faded away.
Jenson was on CPAP for breathing, caffeine to remind his brain to breathe, he was jaundice and had high blood sugar levels.
Day two of being a Mum and I finally got the chance to hold my boy. It was one the happiest day of my life but also one of scariest.
Being given your tiny baby to cuddle was bliss, but you were concerned about how fragile this wee boy was. The tubes and wires were the scariest. The idea that just the slightest movement could knock a tube or wire was terrifying. Your natural instincts hindered by being afraid of hurting your baby by moving your arm and dislodging something.
However as per usual the amazing nurses were so reassuring that Jenson was fine and to just enjoy the moment.
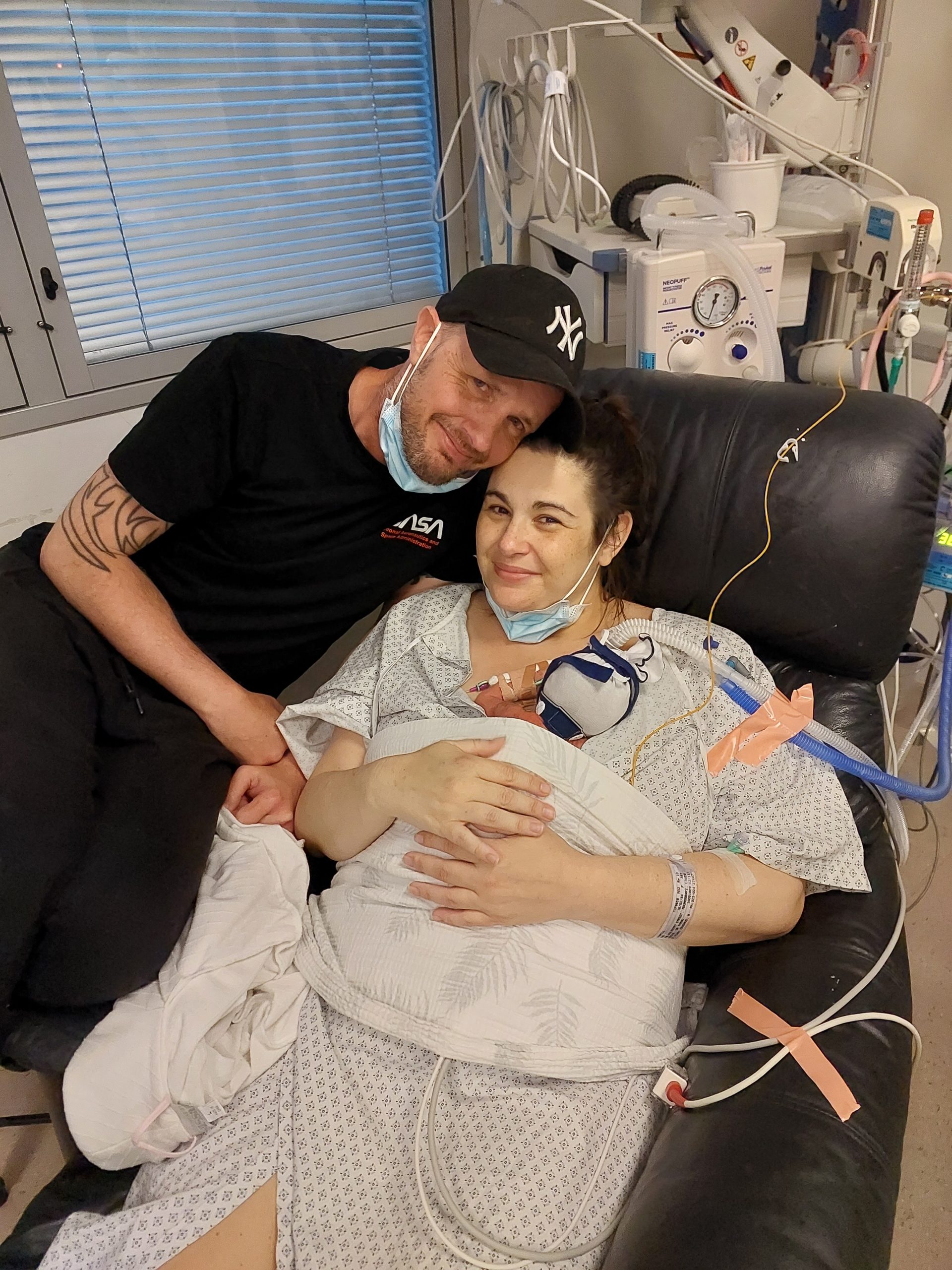
We are so lucky that Jenson was small but strong. He never needed an antibiotic in the first weeks of life, and the doctors main concern was Jensons nutrition, and fat levels on his body. My milk was slow at coming through and we were very lucky to be able to give Jenson donor milk. The appreciation I have for the women who could feed my baby is immeasurable. They could give Jenson the best possible nutritional start that I could not. Our first major road bump was when my partner and I both got covid in the third week of our NICU journey. Jenson was put in isolation as precaution, and the amazing nurses took exceptional care of our boy when we could not be there to give him cuddles and love. We had three video calls a day, which would consist of me crying my eyes out, and being so thankful to the nurse holding the ipad over Jenson for us. Jenson never contracted Covid.
Two days after we were out of isolation we got a call from Jensons nurse, panic sets in as soon as you see the number appear on your phone, panic subsided when we were told Lower Hutt Hospital SCBU had a bed free, and Jenson was strong enough to be moved. Our boy would be only a five minute drive from home, instead of a 20 minute drive if there was no traffic. On the December 2, we said goodbye to the incredible staff of Wellington hospital NICU and were introduced to Hutt Hospital SCBU team.
When we walked into SCBU the first thing I noticed was how intimate it was compared to NICU. All the beds were in the same open plan room, so you could see all the coming and going of SCBU. When Jenson arrived at SCBU he was the oldest baby in the unit and the smallest. SCBU was more laid back to NICU. As it was a smaller unit you got to know the smaller staff and they you and your baby. Jenson being in SCBU also allowed for his grandparents to get to spend more time with their grandson and also that first long awaited cuddle.
Jenson continued to grow and gain weight in SCBU. However a week and a half into our SCBU journey we hit another bump, Jenson started sounding conjested and sneezing. Jenson had contracted RSV. Panic set in again. How was his lungs going to handle it. He was still on low flo oxygen. He was immediately put back into his incubator and all hands on contact ceased. Due to the openness of SCBU, Jensons incubator could only be opened when absolutely necessary so no other babies were infected. After a week of no contact, Jenson was moved into the only isolation room, so we could finally hold him again. In a combination of great doctors and Jensons strength, the virus didn’t hinder Jensons growth or cause any set backs.
With Christmas approaching we were expecting to spending Christmas in SCBU, Jenson was finally being bottle fed and only had his saturation levels being monitored. Then on the 23rd December, Dr Ethan, one of Jensons regular registrars, asked if I was ready to sleep in with Jenson. This meant we were getting to finally bring our boy home.
That night sleeping in with Jenson for the first time was a mixture of emotions. It went well and the night staff were super supportive. I was prepared to stay in another night and wake up Christmas morning in hospital with Jenson, however that morning one of Jensons doctors came in and said the words I had been waiting seven weeks to hear, you can take Jenson home. He was still sneezing a bit, but all his stats were stable and he was gaining weight and taking his bottle well. I hadn’t needed to buy any Christmas presents, as bringing Jenson home was the best gift we could give ourselves and our families.
Jenson left hospital two weeks and two days before his due date and weighing 2.998kg. Since coming home Jenson has thrived. Jenson turned one this month and driving pass Hutt hospital on his birthday, where the journey really began was surreal and emotional.

Having a premature baby changes you. You have to leave your baby each night with people you don’t personally know. You have to trust the staff looking after your baby and know your child is in the best possible hands. The care they provide not just for your fragile child but the care they take in making sure that each baby’s parents are doing ok and coping in this overwhelming situation is incomprehensible and so immensely appreciated by every parent.
The staff at Wellington NICU and Hutt Hospital SCBU are truly earth angels. We are forever indebted to everyone who cared for our Jenson during our most challenging time.
.

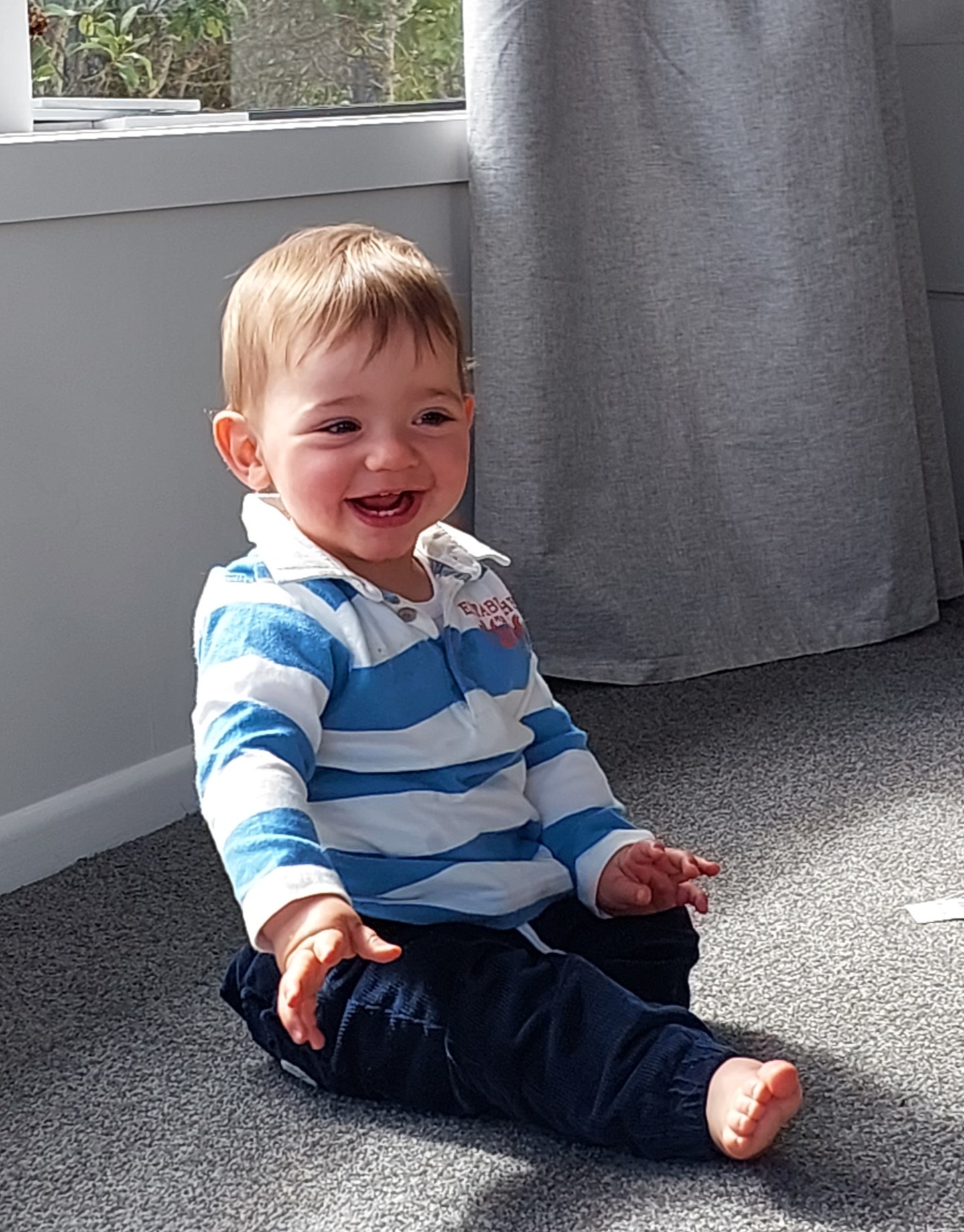
Thanks so much for sharing your personal story Zoe.
We get a lot of positive feedback from families in a neonatal unit who read these stories and feel strength, hope and positivity knowing that they are not alone going through these experiences and feeling certain emotions.
If you would like to discuss sharing the story of your neonatal journey, we’d love to hear from you. Please email info@littlemiraclestrust.org.nz
If you want to help our support of families going through the stress and anxiety of a neonatal journey, you can donate here.
- The Little Miracles Trust provides support to families of premature or sick full-term babies as they make their journey through Neonatal Intensive Care, the transition home, and onwards. We do not receive any Government funding and are entirely reliant on the generosity of individuals, companies and organisations in the form of donations, value-in-kind donations, grants, sponsorship and fundraising events to supplement operating costs and fund our services and initiatives.
- As we are a registered charity (CC56619) with Charities Services New Zealand we will send you an IRD compliant tax receipt – this will happen automatically by return email

