As told by Ginny,
My story starts a little before the twins birth.
Early on in my pregnancy, I got diagnosed with hyperemesis gravidarum, so I was feeling pretty miserable. My husbands boss went on holiday and he ended up working 28 days straight, so I was a single parent to our 10 year old during that time whilst getting fortnightly ultrasounds.
I had found a midwife that I liked, got along with and trusted, but unfortunately, she had to transfer us to the hospital team because there was an abnormal reading for one of our twins. I found this out at 2am when Manage My Health notified me there was a report on the ultrasound, so I paced around the house unable to sleep until 8am. I texted my midwife ‘is there something wrong with 1 of the twins?”, she was just as confused as me as she’d not heard anything either, but eventually found out that there was a minor abnormality but nothing to worry about. She agreed to take care of us postpartum, however, for continuity of care she stated we had to be under the hospital team and also told us that she was available for anything if we needed her.
We switched to the hospital team and had to see the obstetrician and midwife regularly. During one obstetrician appointment I asked for a tubal ligation during the planned c-section (I had to have a c-section because I had previously had one with our oldest) the obstetrician looked past me and asked my husbands for his approval. I wanted a tubal ligation because I was incredibly ill with the twins and didn’t feel like I could go through it again. We eventually got the obstetrician to agree and signed all of the paperwork, everything from there went smoothly until we fast forward to 33+3 weeks.
At 33+3 weeks, I woke up, went to the bathroom and found the mucus plug. I was anxious and called my husband who told me to call the hospital team. At 7am, they told me it was probably nothing but to be safe to come in at 10am for a check. I called my father in law for a ride to the hospital organised for him to look after our eldest while I was at the hospital being checked out.
For the next half an hour, I did my best to try and calm down and then went into planning mode. I packed hospital bags for me and the twins. I simply put them next to the front door as a just in case situation, not actually expecting to need them. My father in law arrived about 10am and dropped me to the hospital then took my eldest to their house.
I went to the maternity ward and told them what had happened. A midwife took me through for monitoring. They checked the twins’ heart rates and monitored me to see if there were any contractions. The midwife sat with me for a few minutes and said it doesn’t look like there are any contractions. She then went off to check on other patients. When she came back, she checked the print off, and I could see her expression change from happy to worried. She abruptly, said “are you in any pain?” I replied with “no, it just feels like braxton hicks contractions”.
The midwife started making calls to the on-call obstetrician, who then came to the labour and delivery room about 45minutes later. The obstetrician told her to give a steroid injection and to get prepared for a vaginal exam plus equipment for a hormone swab. When the obstetrician came in, she had a student with her. It was only when she was doing the vaginal exam that she asked if I was OK with the student doctor being in the room, I agreed as it was already pretty much over. She left the room and came back about half an hour later and said that something had happened with the hormone test and it had to be run again, it should only be a little longer. During this time, the midwife was in and out of the room sitting and talking with me, as well as seeing her other patients. The midwife came back and handed a piece of paper to the obstetrician. She said we’ll there isn’t a lot we can do as your hormones are at 500, I’ll get on the phone about sending you to Wellington, but we will give you the medication to try and stop labour anyway. She proceeded to say I was 2 cm dilated and 80% effaced. I called my husband at work to tell him we were going to Wellington. My husband got to the hospital and was waiting with me for 20 minutes before the ambulance arrived to take us to Wellington.
We arrived at Wellington Hospital around 2.30pm. During the handover, they were all in the room and I felt like they were talking about me as if I wasn’t there. Shortly after I got settled and connected to all of the machines, I asked a midwife where my husband could get some food because he hadn’t eaten since 5am. She kindly brought him a bagged lunch. While he ate, the on-call obstetrician came and said that we were having the babies today, so when the theatre was ready, we would be taken through. My husband stepped out for a 10min walk and a breather. While he was out, they were hooking up iv lines, and bring forms for us to sign.
When the anaesthetist was in the room, I was overwhelmed and started to cry then felt my waters break. The anaesthetist looked at me like I had lost my mind. We went through all the details and medical history, and they brought my husband scrubs to change into. The surgeon came in and had a chat with us, he was lovely and helped lighten the mood. My husband changed, and the surgical team came back to take us through to the operating theatre. They wheeled the bed most of the way when the surgical team realised there wasn’t going to be enough room for baby resuscitation tables, bed, staff and operating table, so they asked if I could walk so I hopped off of the bed and walked into the theatre, and laid on the operating table.
The anaesthetist came in and started the prep to administer the spinal block. While he was attempting to get the spinal block in the correct location, there was shooting pain down my left leg, I alerted him to this as he asked. Once he finally administered the spinal block, I laid down on the bed, and we waited for half an hour, no numbing happened, so the midwifes began monitoring the twins again. We were all chatting and the twins had strong heart beats. Eventually, the senior anaesthetist came in. She helped me to sit up again and started her process of administering the spinal block. The shooting pain in my left leg continued but she managed to get the spinal block in, and she put in an epidural as well for safety as the spinal block was only a half dose.
I lay on the bed and noticed that I was starting to numb out and I had lost control of my bladder. I informed the surgeon, and they inserted a catheter. After all of this, the surgeon said “OK let’s check to make sure a c-section is still viable for the leading twin.” The surgeon got one of the nurses to effectively block the cervix so the leading twin couldn’t escape. They proceeded to do the c-section.
Since they gave me the medication to stop labour, I had a screaming headache, so a lovely gentleman in the operating theatre brought me a cold flannel. The surgeon showed me each of the twins over the drape. They both had a purple tinge to their skin. When I commented on this to my husband, the surgeon reassured me that it was completely normal.
The nurses brought me the smaller twin for a brief cuddle first as she required breathing support (cpap). They then brought me the larger twin for a slightly longer cuddle before taking them through to NICU. While I was having cuddles with the twins, I started to notice breakthrough pain. The breakthrough pain felt like a burning pain in my sternum. I mentioned the pain between baby cuddles, they appeared to not believe me. I asked the nurse to take the larger twin as I was worried about reacting to the pain and hurting one of my babies. Once they took the babies away, my stats started to look odd (resp rate when up, 02 sat’s when down, blood pressure and heart rate skyrocketed) so they gave me pain relief and pushed an epidural.
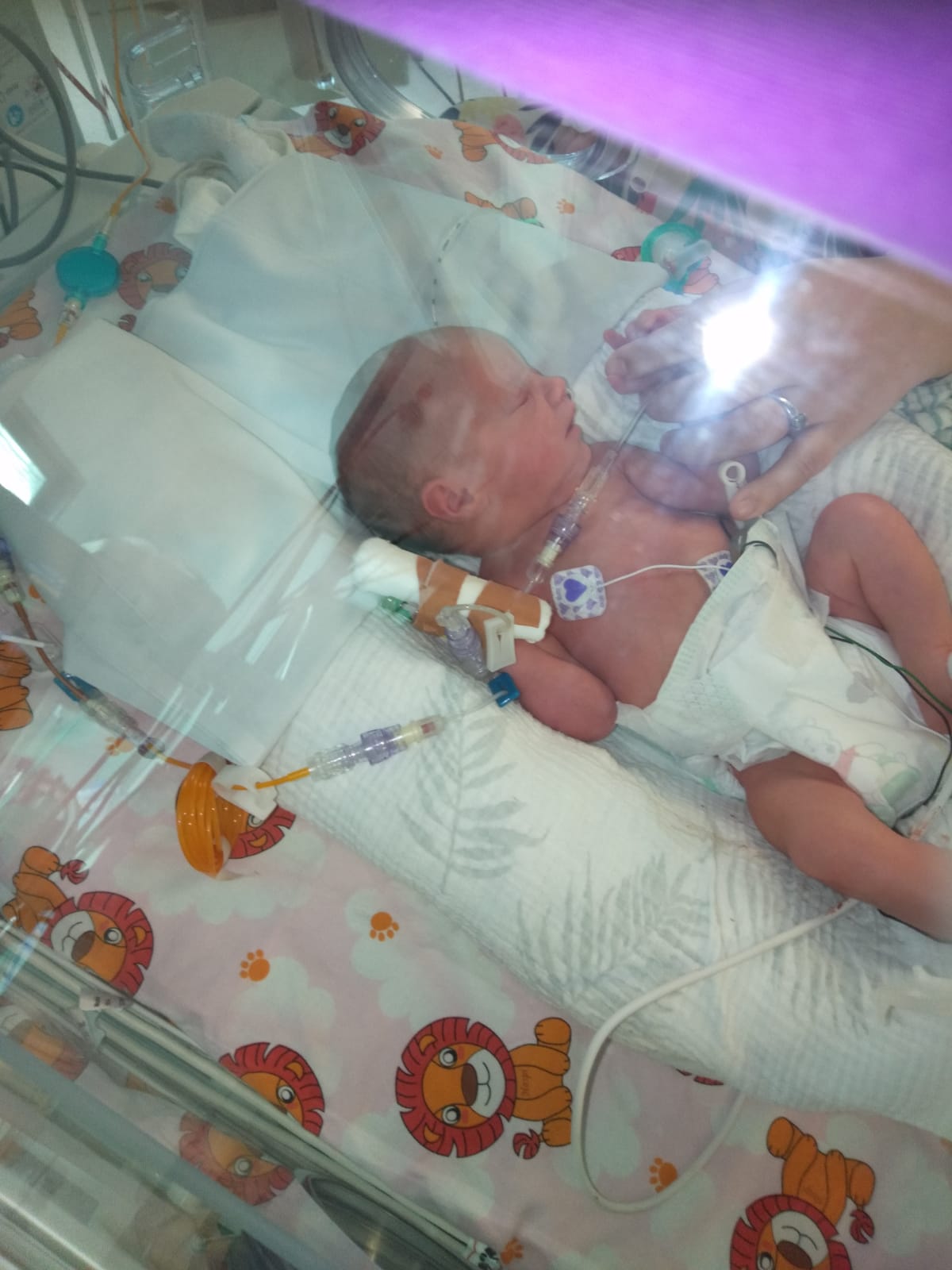
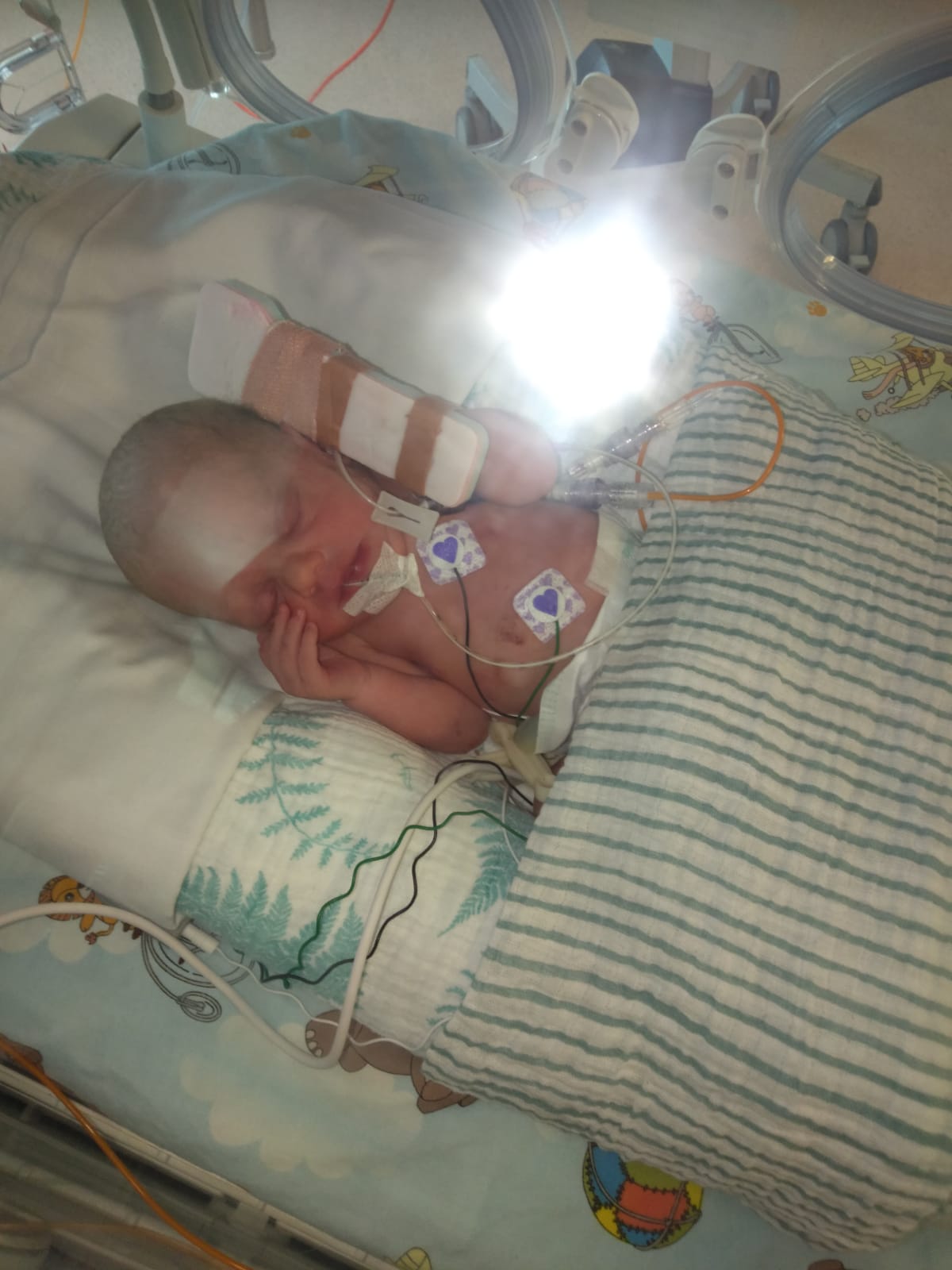
The nurses told my husband that they were taking the twins through to NICU. I could see he was struggling with whether to go with the twins or stay with me. I made the choice for him and said they needed him more than I did, to go, and I would see him in recovery, he gave me a kiss and headed off with the twins.
Once I was all stitched up, they transferred me to a bed, during the transfer they removed the epidural line, and took me through to recovery. The nurse there kept checking on me, and finally brought me a drink of water. At this stage I hadn’t had a proper drink for nearly 12 hours, because of the hyperemesis gravidarum, they were limiting my fluid consumption to make sure I didn’t vomit and tear my stitches.
A short time later, the midwife came back and informed me that she was going to help milk me, to collect colostrum for the twins, I said OK and she proceeded. My husband came through to recovery and gave me an update on the twins, twin A was.1.9 kg, and twin B was 1.8 kg. She was also on cpap, as she was having difficulty breathing.
Once the recovery nurse was content I was stable, the midwife got approval for me to go see the twins in my hospital bed. Being taken into NICU and seeing my babies with all of the tubes and monitors was one of the worst times of my life. I spent what felt like an hour with the twins, held one little hand for a while, and then wiggled to the other side of the bed to hold the other tiny hand. I looked over to my husband, who looked like he was about to pass out from fatigue, so I said to the nurse I was good to be taken to a room. She called the midwife, who came back holding something, she sat it on the foot of the bed and took me to the pods. They were lovely and allowed my husband to stay with me in a pull out bed and gave us sheets, pillow, etc.
Once everything calmed down, I was able to process some of what had just happened, I cried for hours because I blamed myself. Eventually, I couldn’t breathe due to being congested, I wiggled myself towards the edge of the bed to get a box of tissues. I woke my husband up to get a cold cloth for my eyes.
After letting the cloth sit on my eyes for a while to bring down the swelling, I called for the nurse to let her know I had all the feeling back in my limbs and asked her to bring me a wheelchair so I could go see my babies. She said she couldn’t as she was the only one on duty so wouldn’t be able to take me to see them. I looked at her and said the only reason I called her was because I was told a nurse had to see me get up for the first time, basically that I would walk to NICU or my husband could wheel me down, that I just needed her to watch me stand. She was so surprised that I managed to get up without help. My husband took me to NICU, where I found out that Twin B no longer needed cpap. They still didn’t allow me to hold them, but I could hold their hands and look at them, it was great they were side by side so I could hold both of their hands at once.

I spent a couple of hours with them then had a nap for a wee bit. When I woke up, the nurse came through and brought some syringes, she told me that I needed to hand express to get milk for the twins. It all went well but felt stressful because it meant less time with the twins.
I had breakfast, took my medication, and my husband took me to NICU where they still didn’t let me hold the twins but said to come back at 1pm so I could then hold them. So I planned my day around that, had lunch, expressed and was getting ready to go to NICU but the social worker and anaesthesiologist came into check in on us and a few other people visited. It means that by the time I got back to NICU, it was 2.30pm. I found out twin A had jaundice and was under a blue light, so couldn’t hold her. I lost it and started crying, though they allowed me to hold twin B.
I only left NICU for food, toilet, and to express. That night, I asked about pumping rather than hand expressing, the nurse gave a brief overview and left the pumping equipment on the bed and set up the sterilisation bucket while I was in NICU. At about 7pm we went back to NICU, after dinner and pumping…. and both twins were under blue lights, I said to the nurse practitioner that I hadn’t held twin A yet, she said well we have to change that, she got the wonderful nurse Olivia to get twin A out of the incubator and help me get settled but she did say it could only be for 30 minutes or so, at the 30 minute marker the nurse looked me in the eye and smiled, she announced to the room that she was going on lunch, and if we needed anything to let another nurse know, my husband was holding twin B during this time.
The next day was much of the same, I organised for my husband to go hang out with a friend of ours for dinner because he needed a break and time away to reset. I had a schedule that I tried to keep to, so I let the nurses know when I was heading to NICU like I did every time I left, I didn’t register that I hadn’t had my pain relief, so l walked myself to NICU and was there for a while when I started cramping very badly. I got dizzy and had to sit down, started having hot flashes and nausea, the nurses and parents in NICU were watching me closely. I asked if there was a toilet nearby because I had the catheter removed earlier in the day. The toilet for NICU had been closed for renovations, and I had to walk 509 metres to the nearest toilet. It didn’t help, so I went back to NICU and sat with the twins until I realised what was happening. So, I slowly made my way back to the pods and into my room and pressed the call bell, all I was able to say was “pain” to the nurse while crying. I texted my husband because I was hysterical and briefly outlined what had happened. The nurse brought me panadol, ibuprofen, and tramadol. Still in pain, I sat on the edge of the bed for an hour and pressed the call button again, and requested something stronger, by this point my husband was with me. This put the nurse out, and her attitude was rude. When she came back with the pain relief, I apologised for being hysterical. She looked me dead in the eye and said I’d overreacted due to pregnancy hormones, completely ignoring the fact she hadn’t given me pain relief.
On day 3, I walked into NICU to find the radiologist scanning the twins’ heads, looking for brain bleeds… they came up clear, and that was a sign of relief.
I was discharged from the pods on day 4 but they’d organised for me to stay at the Ronald McDonald house across the road. My husband and I decided that he needed to go back to our hometown to be with our eldest child. I was further away from my babies, and my support person wasn’t there anymore, I cried myself to sleep most nights, or I would stay in NICU until I couldn’t keep my eyes open anymore.
The girls were discharged to our hometown, SCBU unit, on day 8. I thought being at home would make it easier to cope but I was very, very wrong. Our eldest wanted to meet the twins but due to covid restrictions, she couldn’t. One day, I got a sign off for her to come in and I called to double check, and was then told that was incorrect, that she couldn’t come in, I had already told our daughter she could meet them. I felt so bad that I ended up laying on the floor sobbing.
The time in our local SCBU was the longest 10 days of my life…. I would go in around 9/10am. I would leave 4/5 pm and come back from 7pm until just before 10pm.
At 36 weeks we were finally discharged, the hospital midwife who was assigned our case came through for the first time, since I went into labour and said look at that, we did good didn’t we?

During SCBU stay the nurses tried put me through to maternal mental health services against my wishes, luckily my midwife stepped in and said that I never agreed to it, but this was after meeting the social worker, who said I was reacting correctly given everything I’d just been through.
Once we were home, it was still a struggle. No-one explained what we should be expecting or the goals we needed to meet but one year on, I am very pleased to say they are both doing great, starting to take their first steps, chatting away between themselves and our paediatrician is extremely happy with their progress.
Happy 1st Birthday to our beautiful twins!

Thanks so much for sharing your personal story Ginny and Happy Birthday to your gorgeous girls!
We get a lot of positive feedback from families in a neonatal unit who read these stories and feel strength, hope and positivity knowing that they are not alone going through these experiences and feeling certain emotions.
If you would like to discuss sharing the story of your neonatal journey, we’d love to hear from you. Please email info@littlemiraclestrust.org.nz
If you want to help our support of families going through the stress and anxiety of a neonatal journey, you can donate here.
- The Little Miracles Trust provides support to families of premature or sick full-term babies as they make their journey through Neonatal Intensive Care, the transition home, and onwards. We do not receive any Government funding and are entirely reliant on the generosity of individuals, companies and organisations in the form of donations, value-in-kind donations, grants, sponsorship and fundraising events to supplement operating costs and fund our services and initiatives.
- As we are a registered charity (CC56619) with Charities Services New Zealand we will send you an IRD compliant tax receipt – this will happen automatically by return email

